In the Cloud: Web 2.0 for T1D management
in Management
It is a common but little-discussed side effect of managing type 1 diabetes (T1D): data overload. Improvements in treatment technologies over the last few decades have made stable glycemic control a much more accessible goal for millions of people. But how to integrate all that technology—combining the data from meters, insulin pumps, and hemoglobin A1c tests, along with exercise and other health information, in a way that you, your family, and your healthcare team can all access, understand, and work with—has remained an unsolved problem. Maybe it’s no surprise that a person living with T1D is solving it now.
Jason Harmon, chief technology officer and founding partner of Get Real Health, didn’t always see himself developing healthcare apps for a living. (In fact, he saw himself in the cockpit of a plane.) But he has harnessed his passion for technology into a successful career that is helping many people, including those with chronic diseases such as T1D.
Get Real Health began as a technology consultancy building custom web applications for companies across many industries. Their focus shifted exclusively to personal healthcare in 2006—back when most hospitals were just beginning to think about digitizing patients’ medical records. That process has since ignited a digital-age revolution in the health-information industry—and Get Real Health is at the forefront. What are they doing that’s so innovative? “We offer patient-engagement software that enables improvement of healthcare outcomes,” Jason says.
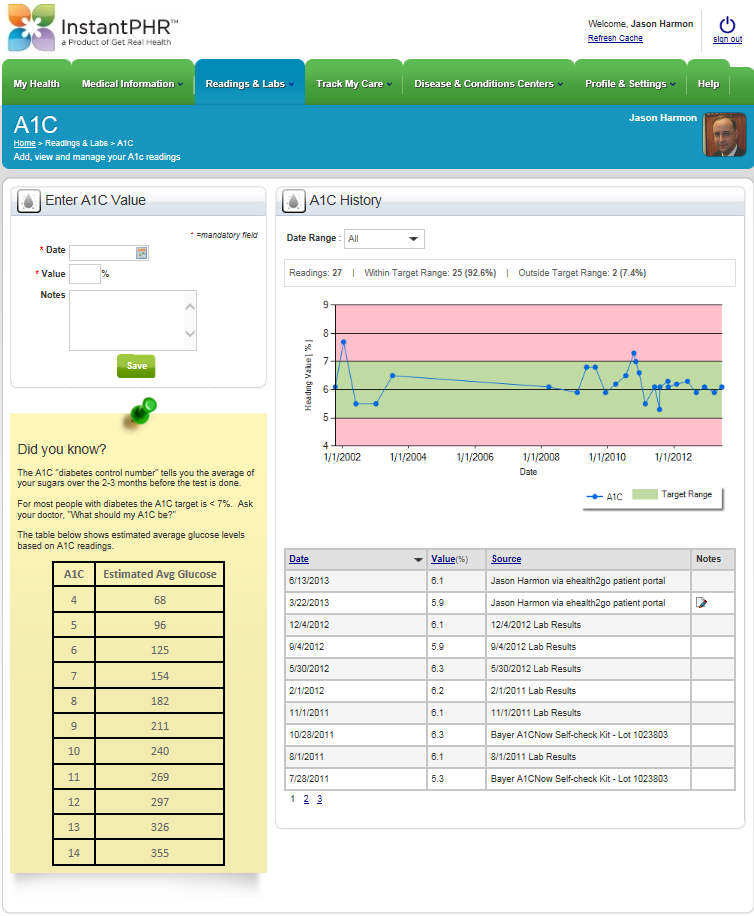 The company’s flagship product is one that Jason himself uses to help manage his T1D. Essentially, InstantPHR (for “personal health record”) is a cloud solution that automatically collects and organizes data from a multitude of medical records, devices, and applications. Patients and physicians can make informed treatment decisions in real time—even when they’re not in the same room. “Being able to see all of that information together allows you to become much better at predicting trends in blood glucose, even against subtler factors like time of year,” Jason says. “It also allows for more effective care, because it allows the clinician access to the wealth of diabetes-management data collected by the patient—which is usually much more than they have in their clinical system—and allows them to see trends that would otherwise be invisible. It lets them see things coming.”
The company’s flagship product is one that Jason himself uses to help manage his T1D. Essentially, InstantPHR (for “personal health record”) is a cloud solution that automatically collects and organizes data from a multitude of medical records, devices, and applications. Patients and physicians can make informed treatment decisions in real time—even when they’re not in the same room. “Being able to see all of that information together allows you to become much better at predicting trends in blood glucose, even against subtler factors like time of year,” Jason says. “It also allows for more effective care, because it allows the clinician access to the wealth of diabetes-management data collected by the patient—which is usually much more than they have in their clinical system—and allows them to see trends that would otherwise be invisible. It lets them see things coming.”
InstantPHR is also highly customizable, with many different widgets and components that can be added depending on how a client will use it. A hospital, for example, may implement a full-feature version, while a private endocrinology practice may be more specific as to what parts it needs.
Introduced in 2009 and validated by case studies performed by several regional healthcare systems, InstantPHR has in a few short years solidified the company’s reputation—enough so, in fact, that Get Real Health is now frequently invited to consult with the U.S. Department of Health and Human Services in an initiative to improve the availability, security, and efficiency of personal medical records. “I think InstantPHR is part of the development that will pave the way for a more patient-centered paradigm in healthcare,” Jason says.
In a holistic turn, it may also eventually help Jason and his fellow pilot advocates win the argument they have upheld for many years—to allow pilots with T1D to fly commercially. “This is a tool that can make it much easier to maintain a detailed history of a person’s type 1 diabetes,” says Jason. “If InstantPHR can help with the effort that gets people with diabetes in the sky—and any other place they want to be—I’d be thrilled.”