Engineering a Better Shield for Beta Cells
Researchers discovered a protein shield that may enhance the protective barrier of encapsulated islets for type 1 diabetes
A new technology for encapsulating islets or beta cells using the human protein called CXCL12 could result in improved encapsulated cell replacement therapies for individuals with type 1 diabetes (T1D). JDRF-supported researcher Dr. Mark C. Poznansky, Associate Professor of Medicine at Harvard, is investigating how CXCL12 could be used to improve the success of implanted encapsulated islets by improving the immune shield around the cells. His initial discovery is published in the March issue of American Journal of Transplantation. Dr. Poznansky began studying CXCL12 more than 10 years ago while working on HIV and ovarian cancer research. He discovered that CXC12 expression on tumor cells has a role in thwarting immune responses against tumors and applied it to T1D islet transplantation research.
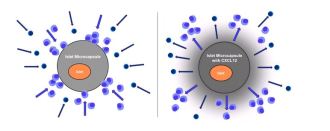
The researcher addresses two challenges with current islet transplantation: 1) T1D patients’ immune systems can readily reject transplanted islets or tissue, and 2) the use of immunosuppressive therapies to combat immune rejection can cause additional health issues for T1D patients. Dr. Poznansky’s new technique involved incorporating CXCL12 into the capsules containing islets for implantation. He found that CXCL12 can induce local immune isolation from the body’s immune system thereby protecting and preserving the long term functions of the encapsulated islets. The protein “shield” tells the attacking immune cells to stay away and keeps them at bay allowing the islets to naturally produce insulin. The majority of the animals receiving islets with the protein shield in the alginate capsule remained healthy and insulin independent for longer than 300 days while those receiving islets with only the capsule all reverted to T1D around day 50. In short, Poznansky designed a technology where a natural protein creates a positive, protective environment for islets or beta cells that could further improve future encapsulated beta cell replacement products for T1D.
A new JDRF grant of $1.6 million will support the team to further their CXCL12-encapsulated cell investigations in additional animal studies. If Poznansky and his team see a good response to the transplants over the first two months, they will proceed with transplanting a second set of animals in a different location and to convey maintenance of islet function long term. Hopefully in the future this “shield” technology will have T1D product applications and constitute part of future generation encapsulation products that help revolutionize the management of T1D.
For more information or to support JDRF’s encapsulation research program, please click here.