#Coverage2Control: JDRF Advocacy to Lower Insulin Prices
By Elizabeth Ransom, JDRF Capital Chapter Communications Committee
At a Senate hearing this spring, a Maine father named Paul Grant described driving to Canada to buy affordable insulin for his son after the U.S. cost soared. This is just one story of how rapid insulin price increases are affecting our communities.
The cost of some insulin has skyrocketed 700% over the past 20 years.
Why are insulin prices rising?
To learn more, I spoke with Jesse Bushman, Senior Director for Health Policy at JDRF. Bushman has worked on drug pricing issues with the federal government, the insurance industry, and with health advocates.
Bushman says this issue is “really complicated,” but explains that it’s important to understand what is driving the insulin prices. “Really it is the rebate driving the price.”
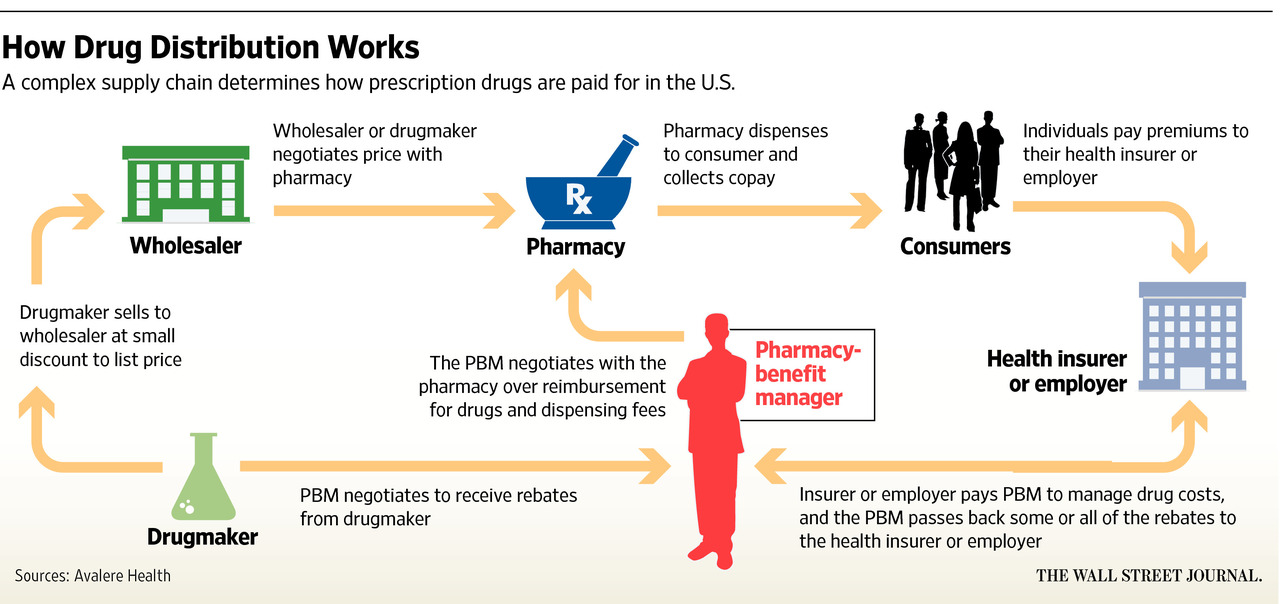
To understand rebates and their powerful influence on insulin prices, it’s essential to grasp how prices are set. This graphic shows various players in the drug distribution process.
Drug makers sell insulin to wholesalers, wholesalers sell to pharmacies, and pharmacies sell to consumers, some of whom pay using health insurance plans. Those plans hire pharmacy benefit managers (PBMs) to negotiate with drug makers to keep drug prices down.
Rebates driving up insulin prices
The three insulin makers—Eli Lilly, Novo Nordisk, and Sanofi—set a “list” price. PBMs determine which drugs will be included in their list of covered drugs, or “formulary.” They demand that insulin manufacturers pay them a significant “rebate”, which in the case of insulin can exceed 70 percent, in return for including the drug on their formulary. So a manufacturer’s “net” price is much lower than their list price. Furthermore, to ensure formulary placement, manufacturers must beat their competition by paying larger rebates. To do that, they must raise prices, which prompts their competitors to raise their prices.
For example, Eli Lilly said between 2012 and 2017 the list price for Humalog increased 215 percent, but the company’s net price increase, after rebates and discounts, was only 13 percent.
Just three PBMs—Optum Rx, CVS Health, and Express Scripts—control the majority of the pharmacy benefit market, so manufacturers are very sensitive to their demands. PBMs typically give a portion of the rebate to insurers, who usually use that money to lower premiums for everyone. The problem with this model is that people who depend on drugs are stuck paying very high (and growing) list prices. Thus, insulin is becoming unaffordable for those without insurance or with high coinsurance or deductibles.
The amount of money PBMs make from rebates is unknown, due to confidential contracts with drug makers. But it’s clear these secretly negotiated rebates play a key role in the rising list price of insulin.
What is JDRF doing about it?
JDRF is leading an advocacy campaign called #Coverage2Control to pressure insurance companies to make insulin more affordable.
Last year, JDRF gathered over 50,000 signatures on a petition urging insurers to drive down out-of-pocket insulin costs. After JDRF shared the petition with 25 insurance companies, United Health and AETNA took steps to begin passing rebates to consumers. Beginning in 2019, they will pass rebates to people they insure, most of whom are covered by small employer plans. They won’t, however, yet pass these rebates to people covered by large, self-insured, employer plans or individual plans.
What can you do?
Now, JDRF is asking for help from the T1D community to send a new message to insurance companies, urging them to pass on the drug savings they receive to their members. The #Coverage2Control site lets you pick your insurer from a list of the largest 25 plans and send them a message. If your company isn’t on the list, there’s a general letter you can modify to send a message to your own plan.
We want to add the patient voice to the discussion and #Coverage2Control enables JDRF volunteers and supporters to advocate directly for changes that will help reduce their insulin costs. So take action today by visiting the site and writing to your insurer!