Types of Insulin You Need To Know (and How They Work)

The Different Insulin Types and How They Work
- Rapid-acting: Rapid-acting insulin starts working about 15 minutes after injection, peaks (or is at maximum effectiveness) in about 1 hour and continues to work for 2 to 4 hours after injection. (Examples: Insulin glulisine (Apidra), insulin lispro (Admelog, Humalog), and insulin aspart (Fiasp, NovoLog)
- Regular or Short-acting: Regular or short-acting insulin starts working 30 minutes after injection, peaks anywhere from 2 to 3 hours after injection, and continues to work for about 3 to 6 hours. (Examples: Human Regular)
- Intermediate-acting: Intermediate-acting insulin starts working 2 to 4 hours after injection, peaks about 4 to 12 hours later, and lasts approximately 12 to 18 hours. (Example: NPH)
- Long-acting: Long-acting insulin is most often combined with rapid- or short-acting insulin. It starts working several hours after injection and tends to lower glucose levels up to 24 hours or almost a full day. (Examples: Lantus, Levemir)
- Ultra long-acting: Ultra long-acting insulin starts working in 6 hours, but it does not peak and lasts about 36 hours, and in some cases longer than that. (Examples: Tresiba, Toujeo)
Ways or Options to Administer Insulin
Injections
Multiple daily injections (also known as MDI or a basal-bolus regimen), involves taking several injections per day. Usually a person will take a basal insulin and then bolus with rapid or short acting insulin when they eat, or their blood sugar is high. Injection sites include the stomach (except for 2 inches near the belly button), the top and outer thighs, and upper and outer arms.
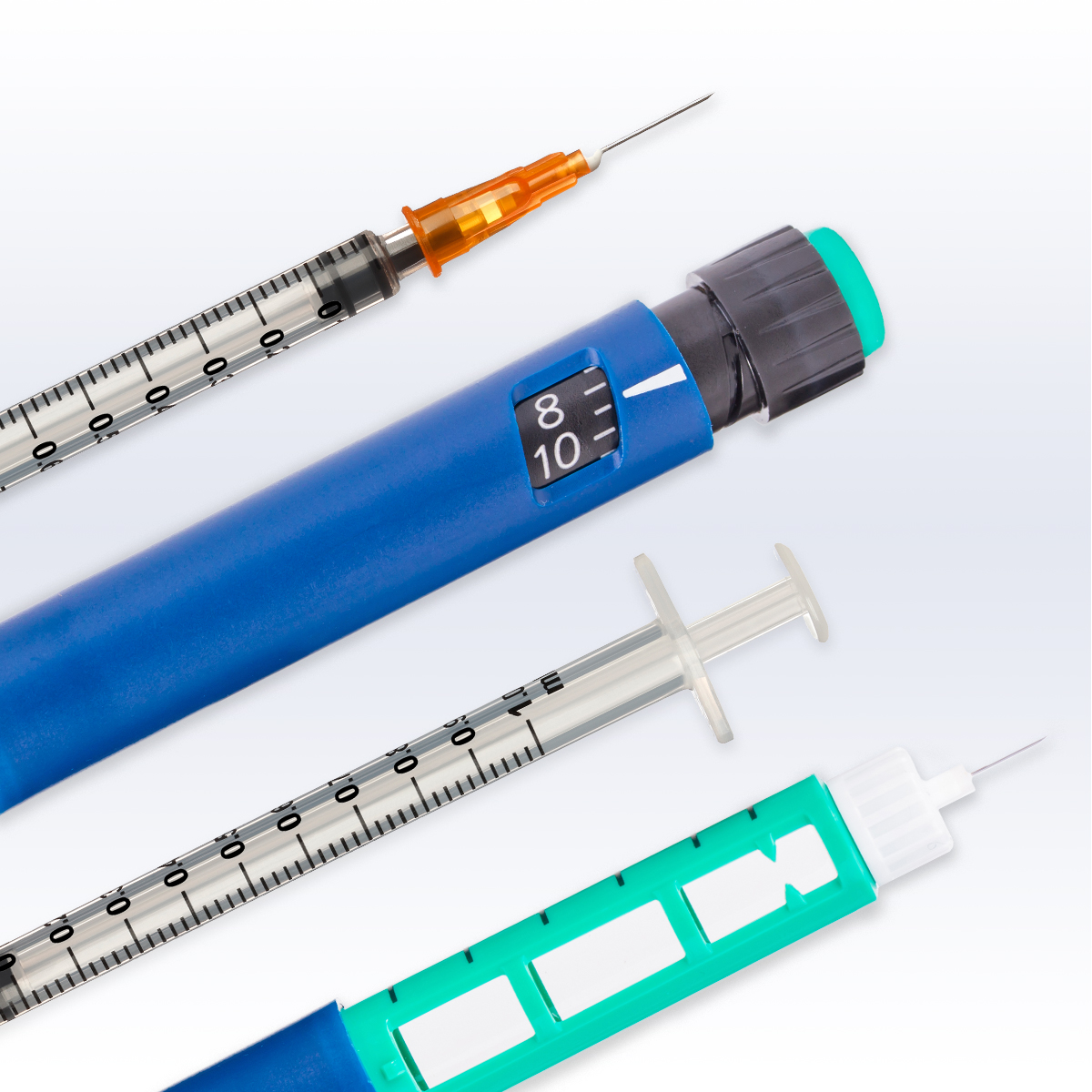
You can inject insulin using insulin syringes and pens. Refer to the device manufacturer’s website or speak with your doctor on how to use insulin syringes and pens correctly and which is right for you. Some people think the pen is more convenient when they only need a single type of insulin, and find pen needles to be more comfortable than syringes. On the other hand, syringes allow you to combine two types of insulin in a single dose and tend to be less expensive than pens.
Pumps
An insulin pump (also known as continuous subcutaneous insulin infusion, or CSII therapy) is about the side of a small cell phone. It delivers small amounts of short or rapid-acting insulin per hour to act as the basal insulin and then when a person eats, or their blood sugar is high, they program in the amount of insulin for the pump to deliver their bolus. Pumps come tubeless or tubed.
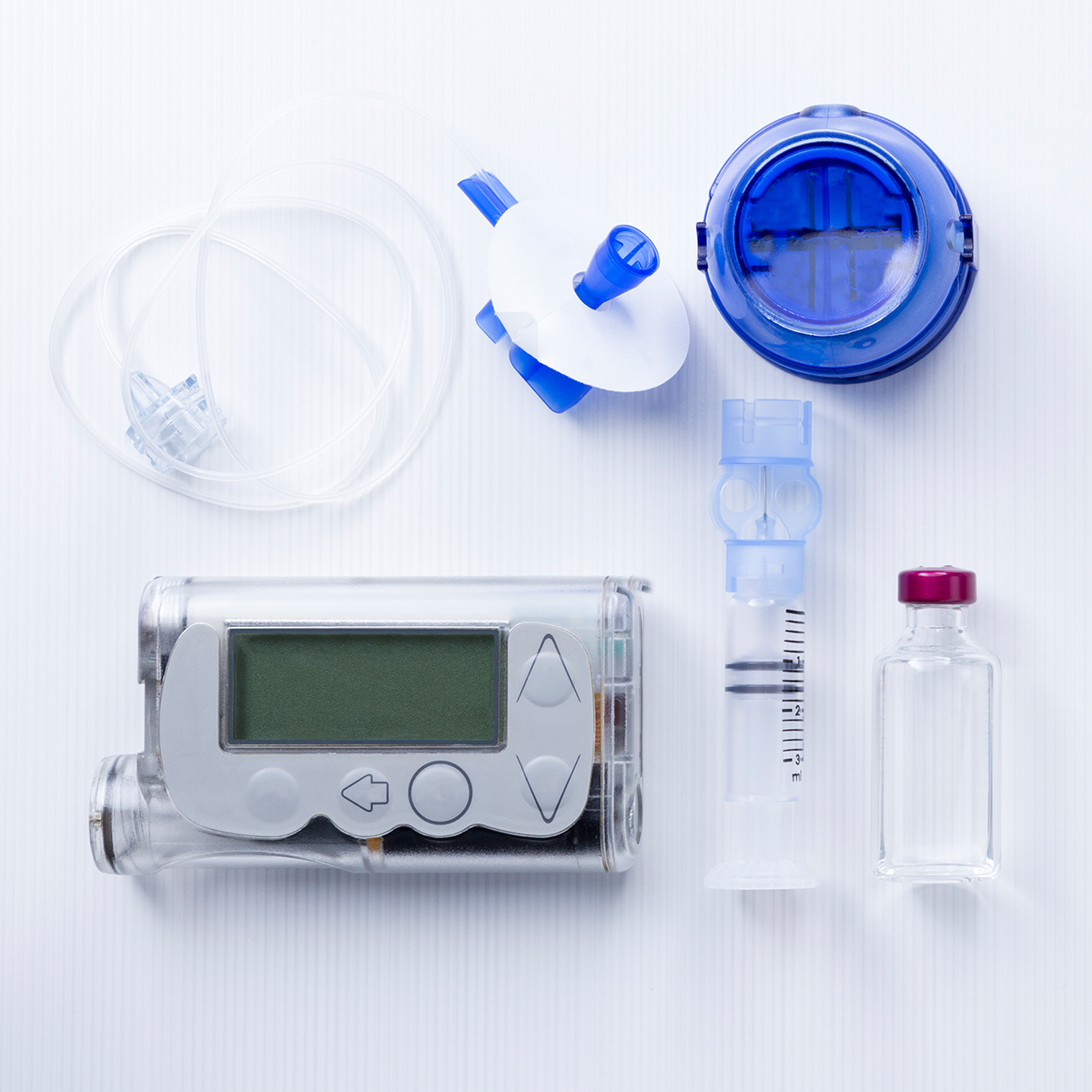
Common pump sites are on the upper thigh, abdomen, along the tricep, and other areas with fatty tissue. The pump is attached to the body using an infusion set, which includes a cannula (a plastic tube), an adhesive, and a small insulin needle inserted into the skin. Once inserted, the cannula is taped in place and the needle is removed. Most pumps have multiple infusion sets that work with them; some are applied manually while others are more automatic. Be sure to explore the options with your health care provider to find the best fit for you.
Inhaled Insulin/Insulin Inhalers
Afrezza, a rapid-acting inhaled insulin, can be an alternative to injectable pre-meal insulin or to cover high blood sugars. It is inhaled immediately before a meal. It is FDA approved for people 18 and over who have type 1 or type 2 diabetes. There are other criteria for use that your physician and diabetes care team can provide.
Lipohypertrophy – Multiple Injections on the Same Part of the Skin
Lipohypertrophy occurs if multiple injections are administered to roughly the same part of the skin over a period of time. When the skin becomes lumpy because of that, and if insulin is injected into the lumpy area, it won’t be absorbed consistently. It would take the insulin longer time to be absorbed, leading to higher than normal blood sugar levels, or can get absorbed too quickly, leading to hypoglycemia. To avoid lumpy skin developing, make sure you pick a different area of skin to put each injection into, also known as rotating your injection site. Ideally, you should aim to keep each new injection spot at least an inch away from your previous injection sites.
Sponsored by
