Cocktail Immune Therapy Beats Going Solo
New clinical results show positive effect of combination immune therapy for type 1 diabetes
Type 1 diabetes (T1D) is caused when the immune system mistakenly attacks insulin-producing beta cells within the pancreas. While there have been numerous clinical studies using general immune therapy to stop or slow the T1D attack, researchers have been generally disappointed with the results.
But data presented at a recent medical meeting suggest a new day may be dawning in the search given clear cut evidence of a benefit from an immune therapy in T1D. Two related studies helped identify a combination therapy approach with new promise in controlling disease progression and possibly reversing the T1D autoimmune process.
One clinical study, funded by JDRF, tested Neulasta, a drug used to reduce the risk of infection in patients receiving strong chemotherapy and the other, funded by JDRF collaborator The Helmsley Charitable Trust, tested a combination of Neulasta and Thymoglobulin, a drug used to suppress the immune system for organ transplants. The goal of both pilot studies was to stop the T1D autoimmune attack and preserve beta cell function in patients with both recent onset and established T1D. The results showed that therapy with Neulasta alone did not help in preserving beta cell function, however combining Neulasta with Thymoglobulin preserved residual beta cell function as measured by C-peptide levels, indicating a slowing of the disease process.
Studies supported by JDRF indicate this combination immune therapy helps restore a better balance among the key immune cells in T1D. The clear demonstration of a beneficial effect from this combination immune therapy in people with established T1D could be the start of a more promising path in immune therapies for the disease. Hopefully, larger clinical trials will bear this out as a next step.
For more information and to support JDRF’s beta cell restoration research program, please click here.
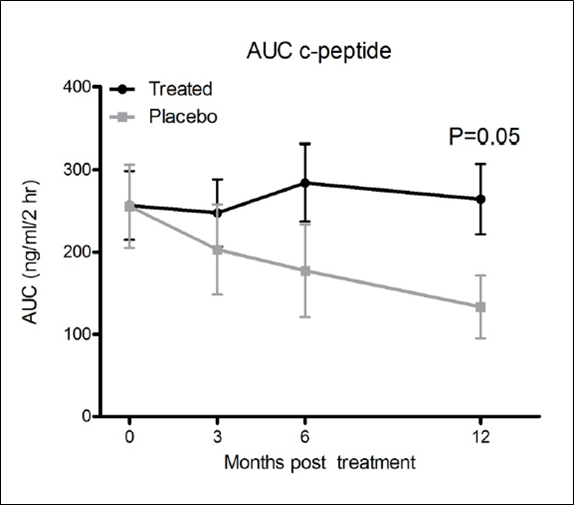
C-Peptide Results of Combination Therapy with Neulasta and Thymoglobin in Recent Onset T1D
Source: ADA 2014 Abstract #173-OR